Archived: Mental health consumers receiving a service within 7 days after discharge from inpatient settings
Persons who receive outpatient services shortly after discharge from an inpatient setting are less likely to require re-hospitalization or crisis services. This emphasis on increasing timely access to local community mental health services supports consumer access to services with better outcomes, is cost efficient, and leads to healthier, safer, and more productive communities.
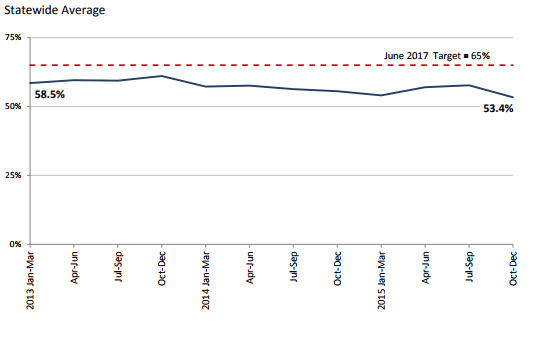
Performance has moderated over the past year – currently at 53.4% in SFQ 2016/2. Although the average time between inpatient discharge and outpatient services has decreased over time, the percentage of consumers receiving no service has increased.
The formal A3 Lean process revealed factors impacting performance:
- A communication gap between the hospital and outpatient treatment provider.
- A lack of outpatient engagement, at both the service delivery level and at the client level.
- The client doesn’t receive immediate help when in outpatient treatment.
- Insufficient training on how to engage clients during the intake process.
Issues (identified in the A3 process) that may impact the ability to engage individuals during the inpatient discharge process include:
- We have a voluntary system. Outpatient appointments might be offered, but individuals decline.
- Inaccurate or contested assignment of hospital stay to a RSN.
- Poor understanding of how to utilize the “Rehab Case Management” modality prevent linkage activities.
- The process of initiating services at a CMHA may be cumbersome and uninviting (e.g., intake assessment).
- Hospitals may fail to alert a RSN of an admission when there is co-insurance.
- The RSN is contracted to offer an appointment occurring within 7 days of discharge, v. the measure calling for a Medicaid enrollee to receive an outpatient service within 7 days of discharge.
Issues with data capture and reporting, and measure definitions (identified in the A3 process) reveal that the measure does not capture:
- Early community provider engagement with clients while in the hospital setting.
- Declines by clients of outpatient appointment offers.
- Appointments occurring within 7 days if the client is rehospitalized within 7 days of discharge.
- Discharges to non-RSN providers (e.g., inpatient AOD treatment, Veteran’s Administration facilities, etc.).
- Services that might be provided but are excluded from the measure definition.
Additionally, data from the “AQM Grant QIP Project: Rehospitalization of Persons with Serious Mental Illness” indicate that the greatest proportion of rehospitalizations occur within 3 days of discharge.
Finally, the metric is a process measure, while Senate Bill 5732 and House Bill 1519 call for DSHS to move to outcome-based measures in its contracts with Behavioral Health Organizations (BHOs).
More Information
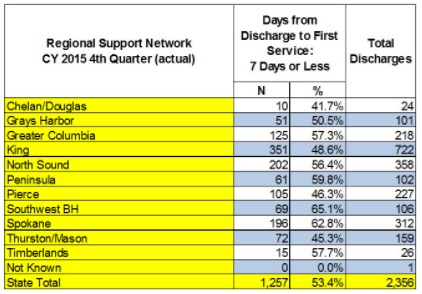
The table is a breakout of metric performance by Regional Support Network for the second quarter of State Fiscal Year 2016 (i.e., the fourth quarter of Calendar Year 2015 [October - December 2015]). The “N” column and “%” column represent the number/percentage of discharges from inpatient services where the number of days from discharge to first outpatient service was 7 or less.
Continue tracking this measure until the new Behavioral Health Services Caseload measure is completed.
The Washington State Behavioral Health Advisory Council (BHAC) has a membership consisting of consumers, providers, advocates, and governmental representatives. The membership represents a balanced representation of the state’s population with respect to race, ethnicity, disability, and age, urban and rural. The Council partners with the Division of Behavioral Health and Recovery to make decisions that will best serve citizens in need of mental health and substance abuse treatment and prevention programs.
You may find more information on BHAC here.